Alpha-Lipoic Acid: Benefits, Side Effects, and Research
Alpha lipoic acid (ALA) was first discovered in 1937, when Esmond Snell found that certain bacteria relied on potato juice to reproduce [1]. This became known as a potato growth factor.
Its first isolation was in 1951 by Lester Reed [2], and its first clinical application occurred in 1959, when German scientists used it to treat liver failure caused by death-cap mushroom poisoning [3].
What is alpha-lipoic acid?
Alpha-lipoic acid (ALA) functions as an essential metabolic co-enzyme, antioxidant, and anti-inflammatory [4]. Physically, ALA is a medium-chain fatty acid with a ring structure on one end that harbors two sulfur atoms.
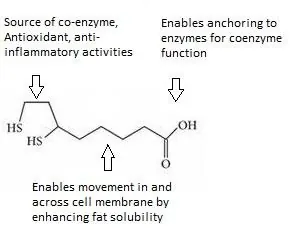 The carboxylate end of ALA, shown on the right side of the molecule, enables it to anchor to proteins to perform as a coenzyme. The left side of the molecule, which has two adjacent sulfur atoms, endows ALA with most of its reactive properties. The central portion of ALA consists of a medium-length carbon chain, which enables ALA to neutralize lipid peroxidation reactions (another form of free radical oxidation) [5,6]. This is unusual when compared to other antioxidants, which are typically either water- or fat-soluble.
The carboxylate end of ALA, shown on the right side of the molecule, enables it to anchor to proteins to perform as a coenzyme. The left side of the molecule, which has two adjacent sulfur atoms, endows ALA with most of its reactive properties. The central portion of ALA consists of a medium-length carbon chain, which enables ALA to neutralize lipid peroxidation reactions (another form of free radical oxidation) [5,6]. This is unusual when compared to other antioxidants, which are typically either water- or fat-soluble.
Alpha-lipoic acid as a co-enzyme
ALA is a non-protein co-enzyme that is bound to numerous protein-based multienzyme complexes. These complexes include the glycine cleavage system and four α-ketoacid dehydrogenase complexes [7].
The glycine cleavage system is responsible for the synthesis of the nucleic acids that make up DNA, RNA, ATP, ribosomes, and other molecules critical to life. The four α-ketoacid dehydrogenase complexes function as parts of the Krebs/citric acid cycle, which transforms energy from carbohydrates, fats, and proteins into carbon dioxide and chemical energy in the form of adenosine triphosphate (ATP). Additionally, the cycle provides numerous amino acid precursors and the reducing agent NADH, which delivers electrons to the electron transport chain to drive the production of ATP [8].
Alpha-lipoic acid’s role in the antioxidant defense system
Exogenous ALA enters cells through the sodium-dependent multivitamin transporter (SDVT), a transmembrane protein responsible for the movement of vitamins and other essential cofactors such as biotin and pantothenic acid [9]. Upon entry into the watery interior of the cell, ALA is reduced by one of several thioredoxin-fold proteins. Reduced ALA is customarily referred to as DHLA. ALA’s antioxidant potential is greatest in this form [10].
ALA interacts with other biomolecules in ways that counter the development of age-related diseases and conditions. These conditions include metabolic syndrome [11,12], diabetes [4], high-blood pressure , atherosclerosis [13], ischemia-reperfusion injury [13], cancer [14,15], and various neurodegenerative disorders [16].
Alpha-lipoic acid and metabolic syndrome
Metabolic syndrome manifests as a constellation of symptoms that include hypertension, insulin resistance, diabetes, obesity, and rising levels of cholesterol and triglycerides. ALA supplementation can lower blood glucose, help reduce obesity, lower blood pressure, and help normalize cholesterol and triglyceride levels [12]. ALA potentially could, and likely does, affect metabolic syndrome as a co-enzyme in energy production, an antioxidant, and an anti-inflammatory.
However, ALA’s most profound effects on metabolic syndrome may be mediated through its reported effects on adenosine monophosphate kinase (AMPK), an enzyme that regulates metabolism based on the ratio of AMP and ATP [11,17]. The difference between AMP and ATP is the two phosphate molecules on the tail:
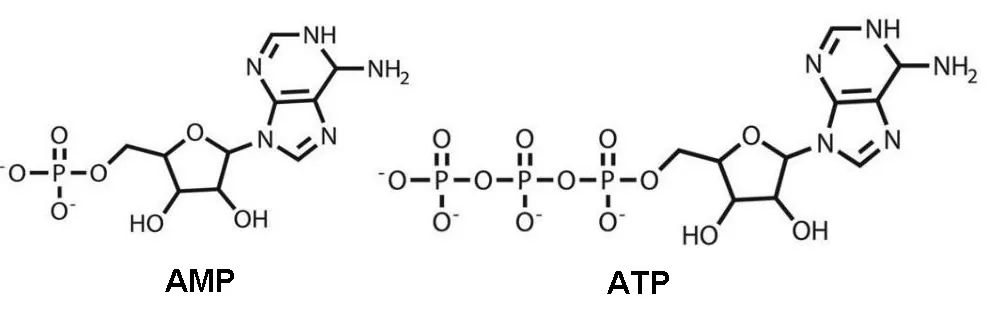
The conversion of ATP to ADP and AMP is what supplies cells with energy, so both of these molecules start to build up during fasting and exercise. AMPK can bind to both AMP and ATP. If AMP binding occurs, AMPK will send out a set of signals that drives the body to use stored energy and put the brakes on cell growth and division. If AMPK binds to ATP, this doesn’t happen. Since there are many AMPs, ADPs, and ATPs, the proportions of each change depending on whether the body is running an energy deficit or surplus.
The role of alpha-lipoic acid
AMPK is affected by many other molecules. ALA has been shown to increase energy expenditure by enhancing AMPK-PGC-1α signaling [17]. PGC-1α is the master regulator of mitochondrial biogenesis {18], and ALA strengthens AMPK’s response to PGC1α to increase mitochondria in skeletal muscle. Increasing mitochondria enables the cell to burn up triglycerides for energy.
Enhancing mitochondrial biogenesis also likely lowers serum triglycerides and cholesterol because the cells’ ability to use triglycerides for energy is enhanced [17]. This also offers an explanation for why ALA would help promote weight loss, as fat is stored triglyceride [19].
Paradoxically, in the hypothalamus, ALA affects eating behavior by inhibiting AMPK, which decreases appetite [20,21].
Alpha-lipoic acid and diabetes
Diabetes mellitus is a multifaceted metabolic disorder in which oxidative stress plays a major role. This has prompted several studies into the use of ALA as a therapeutic adjunct in the treatment of diabetes. In many of these studies, the clearest benefit of lipoic acid supplementation is in patients with diabetic neuropathy [22].
When insulin binds to its receptor, a cascade of reactions occur, leading to the translocation of molecules that transport glucose across the cell membrane. Lipoic acid has been found to activate the insulin signaling cascade in cultured cells [23].
Alpha-lipoic acid and cardiovascular disease
Mechanical and chemical factors, such as hypertension and smoking, inflict oxidative damage on blood vessels, air sacs, and heart muscle in the cardiovascular system.
For instance, chronic hypertension elicits maladaptive changes in how the cells of the heart and blood vessels function [24]. These changes often initiate upwardly spiraling levels of oxidative damage and dysregulation of redox-based cellular communication systems. Evidence suggests that ALA can both mitigate oxidative damage and help resolve abnormalities in redox-based cellular communication. This occurs through multiple mechanisms, including the quenching of free radicals, prevention of T-cell infiltration, restoration of normal calcium and nitric oxide function, and upregulation of genes like ALDH2 that act as system detoxifiers [13].
ALA directly quenches free radicals produced in the cardiovascular system. Additionally, ALA also maintains numerous radical scavenging enzymes, vitamins A,C, and E, and glutathione [25,26]. For example, when a molecule of glutathione quenches a free radical reaction, glutathione becomes oxidized. To reuse glutathione, a more potent antioxidant such as ALA must restore oxidized glutathione to its former state so that it can continue to quench free radicals.
ALA solubility in lipids makes it an antioxidant capable of preventing lipid peroxidation, a process under which oxidants such as free radicals attack lipids containing carbon-carbon double bonds, particularly polyunsaturated fatty acids. Lipid peroxidation is especially important in heart, brain, and nervous system cells. The infrequent replacement of these cells results in their membranes accumulating oxidized lipids [5]. Lipofuscin is an example of lipid peroxidation that is used as an aging biomarker [27]. In fact, ALA has been shown to reduce lipofuscin accumulation in rat brain tissue [28].
ALA reduces T-cell infiltration in atherosclerotic lesions. It is believed that this effect is mediated through the inhibition of vascular cell adhesion molecules (VCAM-1) and intercellular adhesion molecules (ICAM-1) [29,30]. These molecules enable elements of the immune system, such as T cells, to anchor themselves and gain entry to tissues. Short-circuiting the entry of T cells into atherosclerotic lesions prevents additional oxidative damage and the accumulation of macrophage foam cells in the arterial wall.
Foam cells can eventually cause arterial occlusion, resulting in stroke or heart attack [31]. Oxidative damage in this instance is caused by immune cells, which use oxidation to destroy pathogens [32]. Although pathogens are not necessarily a major cause of atherosclerotic lesions, this is a general immune defense mechanism that causes a great deal of collateral damage, particularly when immune activation is chronic in nature.
ALA can aid in the mitigation of drug-induced calcium dysregulation. ALA offsets the side effects of drugs that activate the β-adrenergic receptor. β-adrenergic receptors, when activated, increase cardiovascular, pulmonary, metabolic, and central nervous system activity. This has been shown to increase oxidative stress, heart inflammation, clotting, calcium overload within cardiac muscle, and consequently the risk of heart attack [13].
ALA has been shown to restore endothelial nitric oxide bioavailability and function in the lining of blood vessels. Nitric oxide (NO) relaxes smooth muscles in the arterial wall to lower blood pressure. Additionally, it prevents platelet activation and thereby clot formation. Finally, NO can also decrease blood pressure and cardiac workload by reducing the force of contraction in heart muscle [33].
ALA and DHLA can affect the expression of important genes related to cardiovascular health. Among others, aldehyde dehydrogenase 2 (ALDH2) and Cx3cll play a large role in the overgrowth of cells within the blood vessel wall following injury.
ALDH2 is an enzyme that detoxifies aldehyde compounds in the body [13]. Evidence suggests that ALA and DHLA increase ALDH2, enabling cells to detoxify aldehydes more effectively. Although there is some controversy, it is thought that ALDH2 may help reduce ischemia/reperfusion injury. This is especially relevant in Asian communities, where 40% of the population may carry mutations in the ALDH gene, which lead to unusually high vulnerability to aldehyde toxicity [34,35].
ALA has also been shown to reverse age-dependent changes in CCL2, which recruits immune cells, NFkB, a central mediator of inflammation, and Vcam, which enables immune cells to stick to the inner layers of blood vessels [30,36].
ALA and neurodegenerative disease
ALA has been shown to play a protective role in multiple sclerosis (MS), Parkinson’s disease, Alzheimer’s disease, stroke, and spinal cord injury [16].
ALA is believed to mitigate neurodegenerative disease through multiple mechanisms, including prevention of lipid peroxidation [5], T-cell blockade [30], inhibition of NFkB, and matrix metalloproteinase 9 (MMP), among others [37,38].
Lipid peroxidation is a major threat to brain and nervous system tissue for several reasons. First, neurons are very long-lived cells, so their membranes are subject to long-term damage from accumulating oxidation of the lipid membrane. Second, the fatty acid makeup of brain cells is high in polyunsaturated fatty acids, which are especially vulnerable to oxidation [39]. Third, the breakdown products of lipid peroxidation, often aldehydes, are also toxic to cells [5]. Lipid peroxidation has been implicated in the pathology of Parkinson’s disease and Alzheimer’s disease, among others [40].
MS is an autoimmune disease. Damage occurs because of chronic immune system attacks on the brain and nerves. ALA is believed to alter the expression of cell adhesion molecules, such as ICAM-1 and VCAM-1, in nervous system tissue. This reduces T-cell infiltration, which reduces the infiltration of other components of the immune system that destroy nerve cells [29,30].
ALA also inhibits NF-κB transcriptional activity, which inhibits matrix metalloproteinase 9 (MMP-9) expression in nerve tissue [37,38]. NF-κB is a central mediator in the inflammatory process [41], and MMP-9 plays a special role in nerve and brain tissue.
Extracellular matrix (ECM), the material between cells, has a constantly changing composition. In the nervous system, MMP-9 participates in the remodeling of ECM. This remodeling process includes maintaining myelin, the insulating outer layer of nerve cells that is essential for normal nerve conduction and establishing new neural connections [37].
Dysregulated activation of MMP-9 is implicated in multiple sclerosis [42] along with traumatic brain injury and Alzheimer’s disease [37]. Therefore, ALA may short-circuit the process of neurodegeneration and demyelination. Further, with decreased immune cell infiltration, there is a decrease in ROS production because immune cells actively produce reactive oxygen species as part of their pathogen response mechanism. In short, reducing inflammation reduces oxidation in tissues.
ALA is an antioxidant that is adept at preventing lipid peroxidation, which occurs in cell membranes. Prevention of lipid peroxidation also prevents the accumulation of lipid peroxidation by-products, which include toxic aldehydes such as acrolein [5,43].
ALA treatment in rats following induced strokes was shown to be neuroprotective and facilitated recovery, reducing oxidative damage [44].
Alpha-lipoic acid and cancer
Oxidative stress is linked to tumor development and antioxidants play a critical role in the mitigation of free radical-related diseases. Unfortunately, dosage and bioavailability issues undermine the utility of most antioxidants that might otherwise be useful in cancer treatment. ALA has been shown to exert benefits in patients with advanced cancers by reducing ROS and increasing glutathione peroxidase activity.
In a tissue culture study, ALA was shown to inhibit the growth of breast cancer cells. The research team concluded that ALA inhibited breast cancer cell proliferation and induced cancer cells to self-destruct [45]. More recent studies have looked at ALA delivered in liposomes to improve targeting of cancer cells and bioavailability. In most instances, the inclusion of ALA enhanced the performance of traditional cancer drugs significantly [14].
Alpha-lipoic acid and COVID-19
Oxidative stress is thought to play a role in viral infections. ALA’s antioxidant and immunomodulatory effects are well understood. Consequently, ALA has been tested in several chronic immune diseases [46], and ALA as an adjuvant therapy in COVID-19 patients has a favorable outlook. More precisely, besides reducing oxidative stress and protecting the vascular endothelium, it can diminish the cellular entry of SARS-CoV-2 and inflammation, and it can indirectly stimulate the immune system [47].
Alpha-lipoic acid and longevity
Animal studies show that alpha-lipoic acid prolonged lifespan in certain species [24] but reduced it in progeric mice [25]. There is currently no data supporting such an effects on human lifespan, and studies of the long-term effects on health have not been conducted.
Alpha-lipoic acid side effects
Taken as a supplement, ALA is generally considered safe, with no serious side effects reported. Occasionally, some people may experience mild symptoms like nausea, rashes, and itching. If you experience any serious adverse effects, cease taking ALA immediately and consult your doctor. ALA is commonly found in vegetables such as spinach and broccoli, with smaller amounts found in potatoes, sweet potatoes, Brussels sprouts, peas, and tomatoes. ALA is also found in meats, particularly organ meats, such as the heart, liver, and kidneys.
It is internally produced by some animals, but humans only produce ALA in small amounts. For this reason, it is often sold as a dietary supplement and marketed as an antioxidant.
Disclaimer
This article is only a summary, it is not intended as an exhaustive guide, and is based on the interpretation of research data, which is speculative by nature. This article is not a substitute for consulting your physician about which supplements may or may not be right for you. We do not endorse supplement use nor any product or supplement vendor, and all discussion here is for scientific interest.
Literature
[1] E. E. Snell, F. M. Strong, and W. H. Peterson, “Growth Factors for Bacteria Fractionation and Properties of an Accessory Factor for Lactic Acid Bacteria’,” Biochem, vol. 31, pp. 1780–1799, 1937.
[2] R. L. J., D. B. G., G. I. C., and H. C. S., “Crystalline α-Lipoic Acid: A Catalytic Agent Associated with Pyruvate Dehydrogenase,” Science (80-. )., vol. 114, no. 2952, pp. 93–94, Jul. 1951.
[3] B. Salehi et al., “Insights on the Use of α-Lipoic Acid for Therapeutic Purposes,” Biomolecules, vol. 9, no. 8, p. 356, Aug. 2019
[4] V. Serhiyenko et. al., “Alpha-lipoic acid: mechanisms of action and beneficial effects in the prevention and treatment of diabetic complications,” MOJ Public Heal., vol. 7, no. 4, pp. 174–178, 2018,
[5] A. Catalá and M. Díaz, Editorial: Impact of lipid peroxidation on the physiology and pathophysiology of cell membranes, vol. 7, no. SEP. 2016.
[6] P. Hasanein and A. Emamjomeh, “Chapter 28 – Beneficial Effects of Natural Compounds on Heavy Metal–Induced Hepatotoxicity,” R. R. Watson and V. R. B. T.-D. I. in L. D. Preedy, Eds. Academic Press, 2019, pp. 345–355. doi:
[7] J. A. Mayr, R. G. Feichtinger, F. Tort, A. Ribes, and W. Sperl, “Lipoic acid biosynthesis defects,” J. Inherit. Metab. Dis., vol. 37, no. 4, pp. 553–563, Jul. 2014
[8] G. K. Kikuchi, Y. M. Otokawa,, “Glycine cleavage system: reaction mechanism, physiological significance, and hyperglycinemia,” vol. 84, pp. 246–263, 2008.
[9] M. Quick and L. Shi, “Chapter Three – The Sodium/Multivitamin Transporter: A Multipotent System with Therapeutic Implications,” in Hormones and Transport Systems, vol. 98, G. B. T.-V. & H. Litwack, Ed. Academic Press, 2015, pp. 63–100.
[10] E. Hanschmann et. al., “Thioredoxins, glutaredoxins, and peroxiredoxins-molecular mechanisms and health significance: From cofactors to antioxidants to redox signaling,” Antioxidants Redox Signal., vol. 19, no. 13, pp. 1539–1605, 2013.
[11] M. C. Towler and D. G. Hardie, “AMP-activated protein kinase in metabolic control and insulin signaling,” Circ. Res., vol. 100, no. 3, pp. 328–341, 2007
[12] N. Najafi, S. Mehri, M. Ghasemzadeh Rahbardar, and H. Hosseinzadeh, “Effects of alpha lipoic acid on metabolic syndrome: A comprehensive review.,” Phytother. Res., 2022, doi: 10.1002/ptr.7406.
[13] Q.-F. Hu and A.-J. Sun, “Cardioprotective Effect of Alpha-lipoic Acid and its Mechanisms,” Cardiol. Plus, vol. 5, no. 3, 2020
[14] M. Attia, E. A. Essa, R. M. Zaki, and A. A. Elkordy, “An overview of the antioxidant effects of ascorbic acid and alpha lipoic acid (In liposomal forms) as adjuvant in cancer treatment,” Antioxidants, vol. 9, no. 5, pp. 1–15, 2020
[15] D. P. Tomer, L. D. McLeman, S. Ohmine, P. M. Scherer, B. K. Murray, and K. L. O’Neill, “Comparison of the total oxyradical scavenging capacity and oxygen radical absorbance capacity antioxidant assays,” J. Med. Food, vol. 10, no. 2, pp. 337–344, 2007
[16] H. Khan, T. G. Singh, R. S. Dahiya, and M. M. Abdel-Daim, “α-Lipoic Acid, an Organosulfur Biomolecule a Novel Therapeutic Agent for Neurodegenerative Disorders: An Mechanistic Perspective,” Neurochem. Res., 2022
[17] Y. Wang, X. Li, and Y. Guo, “Alpha-lipoic acid increases energy expenditure by enhancing AMPK-PGC-1alpha signaling in the skeletal muscle of aged mice,” Metabolism, vol. 59, no. 7, pp. 967–976, 2010
[18] H. Liang and W. F. Ward, “PGC-1α: A key regulator of energy metabolism,” Am. J. Physiol. – Adv. Physiol. Educ., vol. 30, no. 4, pp. 145–151, 2006
[19] E. H. Koh et al., “Effects of alpha-lipoic acid on body weight in obese subjects,” Am. J. Med., vol. 124, no. 1, pp. 85.e1-85.e8, 2011
[20] U. Andersson et al., “Exercise in rats does not alter hypothalamic AMP-activated protein kinase activity,” Biochem. Biophys. Res. Commun., vol. 329, no. 2, pp. 719–725, 2005
[21] M.-S. Kim et al., “Anti-obesity effects of α-lipoic acid mediated by suppression of hypothalamic AMP-activated protein kinase,” Nat. Med., vol. 10, no. 7, pp. 727–733, 2004
[22] S. Golbidi, M. Badran, and I. Laher, “Diabetes and alpha lipoic Acid,” Front. Pharmacol., vol. 2, p. 69, Nov. 2011
[23] D. Konrad, “Utilization of the Insulin-Signaling Network in the Metabolic Actions of α-Lipoic Acid—Reduction or Oxidation?,” Antioxid. Redox Signal., vol. 7, no. 7–8, pp. 1032–1039, Jul. 2005
[24] S. Laurent, “https://pubmed.ncbi.nlm.nih.gov/7635546/,” Hypertension, vol. 26, no. 2, pp. 355–362, Aug. 1995
[25] W. Jones, X. Li, Z. Qu, L. Perriott, R. R. Whitesell, and J. M. May, “Uptake, recycling, and antioxidant actions of α-lipoic acid in endothelial cells,” Free Radic. Biol. Med., vol. 33, no. 1, pp. 83–93, 2002
[26] J. Zhang. et al., “Decline in transcriptional activity of Nrf2 causes age-related loss of glutathione synthesis, which is reversible with lipoic acid,” Proc. Natl. Acad. Sci., vol. 101, no. 10, pp. 3381–3386, Mar. 2004
[27] E. Kaemmerer et. al., “Effects of Lipid Peroxidation-Related Protein Modifications on RPE Lysosomal Functions and POS Phagocytosis,” Invest. Ophthalmol. Vis. Sci., vol. 48, no. 3, pp. 1342–1347, Mar. 2007
[28] P. Arivazhagan and C. Panneerselvam, “Alpha-Lipoic Acid Increases Na+K+ATPase Activity and Reduces Lipofuscin Accumulation in Discrete Brain Regions of Aged Rats,” Ann. N. Y. Acad. Sci., vol. 1019, no. 1, pp. 350–354, Jun. 2004
[29] M. Sans et al., “VCAM-1 and ICAM-1 mediate leukocyte-endothelial cell adhesion in rat experimental colitis,” Gastroenterology, vol. 116, no. 4, pp. 874–883, 1999
[30] W. Liu, L. J. Shi, and S. G. Li, “The Immunomodulatory Effect of Alpha-Lipoic Acid in Autoimmune Diseases,” Biomed Res. Int., vol. 2019, 2019
[31] X. H. Yu, Y. C. Fu, D. W. Zhang, K. Yin, and C. K. Tang, “Foam cells in atherosclerosis,” Clin. Chim. Acta, vol. 424, pp. 245–252, 2013
[32] A. Dumas and U. G. Knaus, “Raising the ‘Good’ Oxidants for Immune Protection ,” Frontiers in Immunology , vol. 12. 2021.
[33] T. Heitzer, B. Finckh, S. Albers, K. Krohn, A. Kohlschütter, and T. Meinertz, “Beneficial effects of α-lipoic acid and ascorbic acid on endothelium-dependent, nitric oxide-mediated vasodilation in diabetic patients: relation to parameters of oxidative stress,” Free Radic. Biol. Med., vol. 31, no. 1, pp. 53–61, 2001
[34] J. Zhang et. al.,, “Alpha-Lipoic Acid Ameliorates Oxidative Stress by Increasing Aldehyde Dehydrogenase-2 Activity in Patients with Acute Coronary Syndrome,” Tohoku J. Exp. Med., vol. 229, no. 1, pp. 45–51, 2013
[35] V. Vasiliou and D. Petersen, “4.07 – Aldehyde Dehydrogenases,” (Second E. McQueen, Ed. Oxford: Elsevier, 2010, pp. 131–147.
[36] F. Seifar et al., “α-Lipoic acid, functional fatty acid, as a novel therapeutic alternative for central nervous system diseases: A review,” Nutr. Neurosci., vol. 22, no. 5, pp. 306–316, 2019
[37] S. Reinhard, K. Razak, and I.Ethell, “A delicate balance: role of MMP-9 in Polyunsaturated Fatty Acid Metabolism in the Brain and Brain Cells,” Frontiers in Cellular Neuroscience , vol. 9. 2015.
[38] H. S. Kim et al., “α-Lipoic acid inhibits matrix metalloproteinase-9 expression by inhibiting NF-κB transcriptional activity,” Exp. Mol. Med., vol. 39, no. 1, pp. 106–113, 2007, doi: 10.1038/emm.2007.12.
[39] C. J. E.-C. B.-B. E.-S. L. E.-V. Pallet, “Polyunsaturated Fatty Acid Metabolism in the Brain and Brain Cells,” Rijeka: IntechOpen, 2019, p. Ch. 2.
[40] D. De Araújo et al., “Behavioral and neurochemical effects of alpha-lipoic acid in the model of parkinson’s disease induced by unilateral stereotaxic injection of 6-ohda in rat,” Evidence-based Complement. Altern. Med., vol. 2013, 2013
[41] T. Liu, L. Zhang, and S. Sun, “NF-κB signaling in inflammation,” Signal Transduct. Target. Ther., vol. 2, p. 17023, 2017
[42] A. Trentini et al., “Interplay between Matrix Metalloproteinase-9, Matrix Metalloproteinase-2, and Interleukins in Multiple Sclerosis Patients,” Dis. Markers, vol. 2016, p. 3672353, 2016
[43] K. Nickander, B.Mcphee, P. Low, and H. Tritschler, “Alpha-lipoic acid: Antioxidant potency against lipid peroxidation of neural tissues in vitro and implications for diabetic neuropathy,” Free Radic. Biol. Med., vol. 21, no. 5, pp. 631–639, 1996
[44] C. Lv et al., “Alpha-Lipoic Acid Promotes Neurological Recovery After Ischemic Stroke by Activating the Nrf2/HO-1 Pathway to Attenuate Oxidative Damage.” pp. 1273–1286, 2017.
[45] M.Na, E. Seo, and W. Kim, “Effects of α-lipoic acid on cell proliferation and apoptosis in MDA-MB-231 human breast cells,” Nutr. Res. Pract., vol. 3, no. 4, p. 265, 2009
[46] S. Dragomanova et al., “Therapeutic Potential of Alpha-Lipoic Acid in Viral Infections, including COVID-19,” Antioxidants , vol. 10, no. 8. 2021.
[47] L. Rochette and S. Ghibu, “Mechanics Insights of Alpha-Lipoic Acid against Cardiovascular Diseases during COVID-19 Infection,” International Journal of Molecular Sciences , vol. 22, no. 15. 2021


