Hydrolyzed Collagen: Benefits, Side Effects, and Research
In this article we will be exploring the role of collagens in aging and skin structure.
What is collagen?
Collagens are important structural proteins for the various tissues in our bodies. These include tendon, cartilage, ligaments, blood vessels, muscles, and skin. They act as supporting structures and tether cells together. They give our skin and other tissues its strength and elasticity [1].
They are the most abundant proteins and make up around one-third of all proteins in the body. These are tough, insoluble, and fibrous proteins. Most collagens are tightly packed together to create long, thin fibrils.
What does collagen do?
Various cells produce collagen, but it is mostly produced by connective tissue cells. Collagen is constantly secreted to make sure that tissues maintain their structure. It plays a central role in tissue scaffolding and repair. It is also important in morphogenesis, a process that guides a cell or tissue to develop its shape.
It is present in the extracellular matrix (ECM), a complex network of macromolecules arranged in a cell/tissue-specific way. The parts of the ECM join to form a stable composite, which, in turn, supports tissue form and stability.
The middle layer of our skin (the dermis) is where collagen and fibroblasts form a fibrous lattice. This lattice is a structure upon which new cells can grow, and it allows the replacement of dead skin cells.
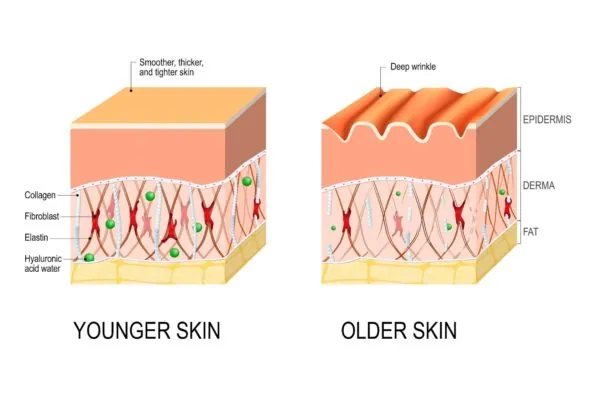
Unfortunately, aging causes collagen production to decline [2]. This means the structure and maintenance of our tissues suffers as a result. The reduced creation of collagen types I and III in particular is typical of aged skin [3].
The most noticeable effect of this decline is in skin health. This progressive loss of collagen as we age causes a loss of skin elasticity and integrity. The result is the formation of wrinkles and weakening of joint cartilage. In women, there is a significant loss of collagen following menopause [4].
Types of collagen
There are 28 collagen proteins in humans, denoted using Roman numerals from I to XXVIII. While this may sound like a lot, between 80 to 90 percent of these belong to types I, II, and III. We will be mostly focusing on these three types of collagen in this article.
Types I, II, and III are fibrillar collagens from the same family. This means they are made of separate collagen proteins bundled into large fibers. These bundles then provide strength and support to tissues.
Collagen I is found in the connective tissues of tendons, ligaments, bone, skin, and corneas. Collagen II is mostly present in cartilage tissue. Collagen III can be found in skin and blood vessels.
Medical and cosmetic uses
Collagen is used as a way to help heal wounds. It promotes healing by attracting new skin cells to the wound site. Its presence creates a structure upon which these new cells can grow and so helps heal wounds faster.
The use of collagen dressings to heal chronic wounds, necrotic wounds, second degree burns, and skin graft sites is also common.
Collagen-based membranes are used in dental surgery to prevent gum cells travelling to a tooth injury. This is to stop them taking the place of slower growing tooth cells. Doing this gives the slower cells time to regenerate the tooth. There are also sutures made from collagen used for dental and ophthalmologic surgery.
In all of these uses, collagen-based membranes are resorbable by the body. This means that they will be broken down naturally and do not need to be removed.
What is hydrolyzed collagen?
Hydrolyzed collagen is made by breaking down collagen into its component amino acids and peptides. To achieve this, enzymes such as those produced by the pancreas or other digestive organs. Heat exposure is another way to create hydrolyzed collagen.
Type I to III collagens are frequently hydrolyzed and made into supplements. These have potential in improving skin structure, reducing joint pain, and improving hypertension.
Collagens I to III primarily contain the amino acids hydroxyproline, glycine, and proline. However, there are differences in the numbers and types of peptides each contains. Unfortunately, at this time, the studies comparing each type and source of collagen are yet to be done.
Sources of collagen
Endogenous collagen is made by your body, but the exogenous variety is synthetic and comes from an outside source, such as supplements. It is used in some medical procedures and supplementation with collagen is used for cosmetic purposes. Exogenous collagen comes from various species, including cows, chickens, pigs, fish and shellfish.
Marine collagens are the better option if there is a choice between it and bovine/avian collagen. This is because there is a lower risk of inter-species disease transmission from marine species.
Diseases such as mad cow disease or avian or swine flu are a potential concern with collagen. Yet, hydrolyzed collagen from bovine, swine, avian, and marine sources have not shown any safety concerns in clinical trials.
There have been a few human studies where hydrolyzed collagen shows promise.
Hydrolyzed collagen for skin aging
As mentioned earlier, collagen production declines progressively as we age. From around the age of 18 or so, its production steadily declines at a rate of roughly 1% every year [6].
Cosmetic collagen creams are often marketed as being able to address skin aging, but the evidence for this is weak. Regular collagen cannot penetrate the skin, though its hydrolyzed form can likely enter the top layer of skin due to its smaller size. This means that such creams cannot replace lost collagen deeper down in the skin layers, although they may improve skin moisturization.
However, oral supplementation of hydrolyzed collagen has shown some promise against skin aging. The results of a small study of 69 women aged 35-55 years old suggest that supplementation may improve skin elasticity [7].
The participants were given either 2.5 or 5 grams of hydrolyzed collagen or a placebo daily for a period of 8 weeks. Both doses of hydrolyzed collagen improved skin elasticity between 4 to 8 weeks by around 7 percent. There was no real difference between either dosage group, as both saw similar improvement compared to the placebo group.
One study, involving 112 women who were 39 to 59 years old, investigated its influence on skin aging [8]. One group was given 300 milligrams of hydrolyzed collagen, 50 milligrams of hyaluronic acid, and 100 milligrams of chondroitin sulphate. The other group was given a placebo containing 500 milligrams of cellulose. This was taken twice daily for a period of 12 weeks.
Both groups had significant improvement in skin dryness, skin texture, smoothness, and skin tone, but the collagen group did better than the placebo group when it came to reducing facial lines and wrinkles.
In another trial, 64 female participants were given a liquid supplement containing 100 milligrams of vitamin C and 3000 milligrams of fruit concentrate [9]. The test group also had 1000 milligrams of hydrolyzed collagen added to this supplement. This was taken once a day for a period of 12 weeks. Participants could also use topical cosmetics supplied by a specific company.
The test group showed 7.23-fold greater skin hydration at the 6-week mark. This fell to 2.9-fold at 12 weeks compared to the placebo group.
There was a reduction of the visual grade for wrinkle formation. At 12 weeks there was a significant improvement compared to before the study began in the test group. There was a 10.5-fold improvement in the test group compared to the placebo. Finally, the elasticity of the skin was greater in the test group versus the placebo.
The improvement at 12 weeks in the placebo group was likely due to the vitamin C and fruit concentrate or the topical cosmetics. Allowing topical cosmetics muddied the water, but there was still a clear difference between the test and control groups.
Hydrolyzed collagen for rheumatoid arthritis
A study of 274 participants between 18 and 80 years old suggested that hydrolyzed collagen may improve the condition [10]. The results suggest that it could reduce the stiffness and pain associated with rheumatoid arthritis.
Participants were given either a 20-, 100-, 500-, or 2500-microgram dose of type II hydrolyzed collagen or a placebo. This was given daily for a period of 24 weeks. The study participants were not allowed to use other drugs for their condition.
39 percent of the participants given 20 micrograms of hydrolyzed collagen saw improvement of their Paulus criteria. This was versus 19 percent in the placebo group. The same group also improved on the American College of Rheumatology criteria. There was a 30 percent fall in tender and swollen joint scores versus placebo.
The higher doses did see improvements, but they were not statistically significant. There was no real difference in response rates between the four doses used.
A study of 503 participants suggests that hydrolyzed collagen may be useful [11]. Participants took 100 micrograms of type II daily for a 24 week period. The results were compared to another group taking 10 milligrams of rheumatoid arthritis drug methotrexate for the same duration.
Both groups saw significant reductions in pain, joint tenderness, swollen joint totals, and morning stiffness. However, the methotrexate group did better in all these criteria than the collagen group.
C-reactive protein, a biomarker of inflammation, had dropped by roughly 11 percent in the collagen group by week 24. Methotrexate clearly performed better, with a reduction of 35.1 percent by the week 24 mark.
While methotrexate did outperform the collagen, it does show that as a treatment, it had merit. Further studies using different types of collagen and from more sources should be conducted. It would also be interesting to see if a drug such as methotrexate has synergistic effects when combined with hydrolyzed collagen.
Hydrolyzed collagen for osteoarthritis
A trial of 80 people used a commercial product containing hydrolyzed collagen to explore its influence on osteoarthritis [12]. Participants were given a commercial product containing 600 milligrams of type II hydrolyzed collagen, 200 milligrams of chondroitin sulphate, 100 milligrams of hyaluronic acid, and 50 milligrams of unspecified cartilage components. The placebo group was given a 1-gram solution containing cellulose.
These were taken twice a day for a period of 70 days. Participants were not permitted to use anti-inflammatory drugs, corticosteroids, or drugs that suppress the central nervous system.
At the end of the study, the researchers evaluated the pain levels of participants using a visual analogue scale. Both groups showed significant reductions in acute and chronic pain compared to their pre-study baselines. The big difference was that the commercial product reduced pain scores 35 percent versus 14.9 percent for the placebo.
On the Western Ontario and McMaster Universities Osteoarthritis Index, the commercial product reduced pain scores by 38 percent. The placebo group also saw improvement but only 19.8 percent.
Hydrolyzed collagen for type 2 diabetes
A study involving 100 participants with T2 diabetes and hypertension, plus 50 healthy people, looked at its potential for treating this disease [13]. Participants were given 6.5 grams of marine hydrolyzed collagen or 6.5 grams of the placebo carboxymethylcellulose.
This was taken twice a day for a period of three months. During the study, participants were allowed to take prescription antidiabetic and antihypertensive drugs. Both groups were also given educational instruction relating to diet and exercise.
The collagen group had a 19.7 percent reduction of fasting blood glucose levels at the 3-month mark versus their baseline scores. The placebo group only saw a 3 percent improvement. They also showed a significant reduction in HbA1c, a biomarker for long-term blood glucose levels and control. HbA1c fell by 6.8 percent compared to baseline versus 1.7 percent for the placebo group.
Systolic blood pressure was reduced in both groups, but only the collagen group saw a fall in diastolic blood pressure equalling 5.7 percent. Finally, there was a significant reduction of triglycerides, cholesterol, low-density lipoprotein, and free fatty acids, plus a rise in high-density lipoprotein in the collagen group versus baseline.
The addition of dietary and exercise education may well have influenced the data during this study; however, there was still a clear difference between test and placebo groups. This suggests that marine hydrolyzed collagen could be a useful supplement in the context of T2 diabetes.
Collagen side effects
Oral collagen supplements may cause side effects, including a bad taste in the mouth, heartburn, and a feeling of fullness or bloating.
Disclaimer
This article is only a very brief summary, is not intended as an exhaustive guide, and is based on the interpretation of research data, which is speculative by nature. This article is not a substitute for consulting your physician about which supplements may or may not be right for you. We do not endorse supplement use or any product or supplement vendor, and all discussion here is for scientific interest.
Literature
[1] Kadler, K. E., Baldock, C., Bella, J., & Boot-Handford, R. P. (2007). Collagens at a glance. Journal of cell science, 120(12), 1955-1958.
[2] Ryazanov, A. G., & Nefsky, B. S. (2002). Protein turnover plays a key role in aging. Mechanisms of ageing and development, 123(2-3), 207-213.
[3] Varani, J., Dame, M. K., Rittie, L., Fligiel, S. E., Kang, S., Fisher, G. J., & Voorhees, J. J. (2006). Decreased collagen production in chronologically aged skin: roles of age-dependent alteration in fibroblast function and defective mechanical stimulation. The American journal of pathology, 168(6), 1861-1868.
[4] Hall, G., & Phillips, T. J. (2005). Estrogen and skin: the effects of estrogen, menopause, and hormone replacement therapy on the skin. Journal of the American Academy of Dermatology, 53(4), 555-568.
[5] Rodella, L. F., Favero, G., & Labanca, M. (2011). Biomaterials in maxillofacial surgery: membranes and grafts. International journal of biomedical science: IJBS, 7(2), 81.
[6] Baumann, L. (2007). Skin ageing and its treatment. The Journal of Pathology: A Journal of the Pathological Society of Great Britain and Ireland, 211(2), 241-251.
[7] Proksch, E., Segger, D., Degwert, J., Schunck, M., Zague, V., & Oesser, S. (2014). Oral supplementation of specific collagen peptides has beneficial effects on human skin physiology: a double-blind, placebo-controlled study. Skin pharmacology and physiology, 27(1), 47-55.
[8] Schwartz, S. R., Hammon, K. A., Gafner, A., Dahl, A., Guttman, N., Fong, M., & Schauss, A. G. (2019). Novel Hydrolyzed Chicken Sternal Cartilage Extract Improves Facial Epidermis and Connective Tissue in Healthy Adult Females: A Randomized, Double-Blind, Placebo-Controlled Trial. Alternative therapies in health and medicine, 25(5), 12–29.
[9] Kim, D. U., Chung, H. C., Choi, J., Sakai, Y., & Lee, B. Y. (2018). Oral intake of low-molecular-weight collagen peptide improves hydration, elasticity, and wrinkling in human skin: a randomized, double-blind, placebo-controlled study. Nutrients, 10(7), 826.
[10] Crowley, D. C., Lau, F. C., Sharma, P., Evans, M., Guthrie, N., Bagchi, M., Bagchi, D., Dey, D. K., & Raychaudhuri, S. P. (2009). Safety and efficacy of undenatured type II collagen in the treatment of osteoarthritis of the knee: a clinical trial. International journal of medical sciences, 6(6), 312–321. https://doi.org/10.7150/ijms.6.312
[11] Wei, W., Zhang, L. L., Xu, J. H., Xiao, F., Bao, C. D., Ni, L. Q., … & Wang, R. C. (2009). A multicenter, double-blind, randomized, controlled phase III clinical trial of chicken type II collagen in rheumatoid arthritis. Arthritis research & therapy, 11(6), 1-10.
[12] Schauss, A. G., Stenehjem, J., Park, J., Endres, J. R., & Clewell, A. (2012). Effect of the novel low molecular weight hydrolyzed chicken sternal cartilage extract, BioCell Collagen, on improving osteoarthritis-related symptoms: a randomized, double-blind, placebo-controlled trial. Journal of agricultural and food chemistry, 60(16), 4096-4101.
[13] Zhu, C. F., Li, G. Z., Peng, H. B., Li, Y., Zhang, F., & Chen, Y. (2010). Therapeutic effects of marine collagen peptides on Chinese patients with type 2 diabetes mellitus and primary hypertension. The American journal of the medical sciences, 340(5), 360-366.