The world is currently experiencing a period of rapid population aging, with estimates stating that by 2050, about 22% of the global population will be aged 60 years or older; by the end of this century, that percentage might be potentially as high as 33%. This trend is so pronounced worldwide and so impactful that it is called the “silver tsunami”. Some countries are experiencing even faster population aging, such as Japan, where the share of people aged 65+ has already reached 26.3% and is estimated to be close to 40% by 2050 [1].
The morbidity structure of the population is changing accordingly: chronic age-related diseases have become the leading causes of disability and death in developed countries, and developing countries are quickly catching up.
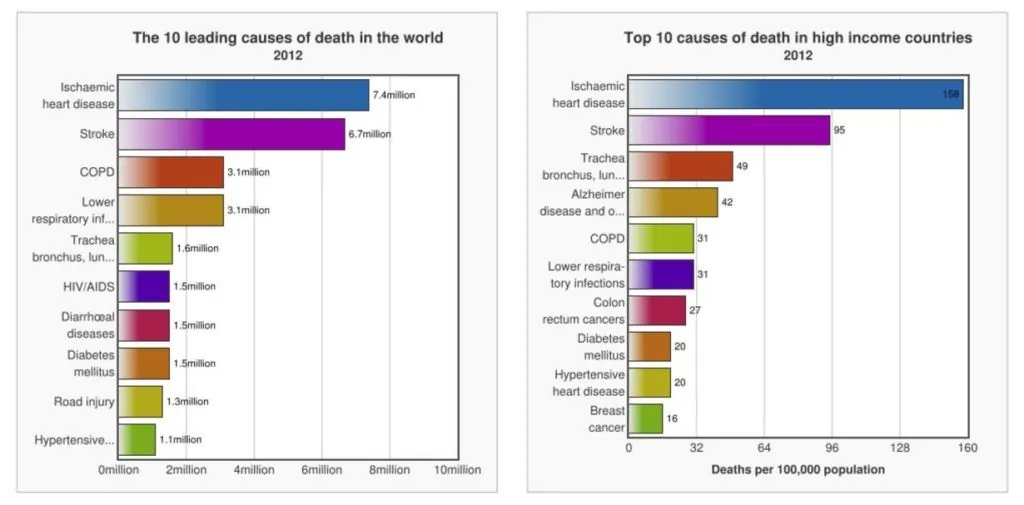
Fig 1. The 10 leading causes of death in the world 2012. Top 10 causes of death in high income countries 2012. Source: WHO Media Centre.
Health care expenditures increase, and a shrinking workforce provides fewer resources to support the elderly. The old age dependency ratio (number of people aged 65+ by 100 people of working age) is also increasing worldwide. For instance, in the United States, the old-age dependency ratio, which was 22.3% in 2015, is estimated to increase to 36.9% in 2050 and could reach 47.9% by 2100 [1]. Currently, each American retiree is supported by 4 other people; by 2100, there will only be 2 helpers providing for their needs.
Recent studies in the EU (a region experiencing very fast population aging) show that higher old-age dependency ratio is related to lower income per capita growth over the last two decades. The researchers assume that there are potential negative effects of population aging on the future economic growth of Europe [2] – which may be the same for all other countries with a similar demographic profile.
Even though increasing life expectancy is certainly a great achievement of humanity, its consequences, such as a proportionally reduced workforce and the increasing morbidity of age-related diseases, create a number of risks for the economy. We cannot ignore this trend, and we must undertake a number of measures to ensure sustainable development of the global society in the medium to long term.
But who is going to deal with the increasing needs for caregiving?
According to the U.S. Department of Labor, women make approximately 80% of the health care decisions for their families, and they are also more likely than men to be caregivers to family members [3-5]. An American Academy of Family Physicians (AAFP) national survey (2008) has found that around 90% were responsible for health care decision-making for themselves and/or family members [6]. Women are more likely than men to play a role of primary family caregiver. For older adults, about two-thirds of caregivers are women [7].
Stakeholders in the field of elderly caregiving in the United States also report a deficiency of elderly care specialists and facilities, which is going to become worse in the future as the population ages and the workforce diminishes. Therefore, it is very likely that most of the burden related to nursing the disabled elderly will be placed increasingly on the shoulders of women, in both paid and unpaid (family) caregiving.
We can see it happening in modern Japan. The current old-age dependency ratio in this country (number of old people by 100 workers) is the highest at 43.3 and is estimated to reach 70.9 by 2050, which means that four workers will need to support three elderly people [1].
In a recent study, it was shown that women traditionally play the main role in caregiving in Japan, making nearly 80% of all caregivers. As the burden of caregiving has been increasing due to population aging, the government introduced a program of long-term care insurance (LTCI) to provide formal care with a 10% co-payment, based solely on a functional assessment of the recipient. As a result, the share of traditional female caregivers decreased from 78.2% to 68.6%, while male caregivers increased their participation. However, this also created higher risks of maltreatment for care recipients (because of the lack of skills for caregiving in men) [8].
So, if we use Japan as a prototype of what will happen to caregiving in developed countries, we can expect, as a result of the introduction of governmental support programs, that the amount of male caregivers will increase but the female caregiver group will still carry most of the burden on their shoulders.
That is not all. One of the solutions for population aging that is being actively promoted by different stakeholders is the increase of the birth rate; countries such as China, Japan, Vietnam, Italy, Spain, and others facing fast population aging are undertaking measures to encourage reproduction. The goal of these efforts is to bring balance in regards to population age, as more births will mean more young people who can enter the workforce.
The problem here is that the generation encouraged to procreate is also the same generation needed to increase their support for the elderly. As both children and elderly require care, based on the above statistics, this stands to place a potentially intractable burden on women in the years to come. It might indeed become much harder to live your life the way you want in 2050 if you are a woman.
Luckily, there is a solution; rather, there might be a solution, if women will help to create it. This solution is to increase support for research on aging and longevity. By helping the scientists developing effective treatments to slow down, arrest, and eventually reverse age-related damage, we can help prevent chronic age-related diseases.
 The burden of cancer, cardiovascular diseases, osteoarthritis, hearing and vision loss cause a great deal of suffering to the elderly and are often the reason why people become disabled and dependent on their families. If such technologies are available to most of the population in middle age, it could help extend the period of peak health, enabling the elderly to avoid disability and to be independent and productive for longer periods of time.
The burden of cancer, cardiovascular diseases, osteoarthritis, hearing and vision loss cause a great deal of suffering to the elderly and are often the reason why people become disabled and dependent on their families. If such technologies are available to most of the population in middle age, it could help extend the period of peak health, enabling the elderly to avoid disability and to be independent and productive for longer periods of time.
Science is increasingly showing that the processes of aging are manageable, but to cope with the pace of the “silver tsunami”, we need to increase our support for research on aging now.
For women, this is a win-win investment, whether they are taking part in crowdfunding for aging research or joining rejuvenation biotechnology startups as business partners. If the various aging processes can be brought under medical control, women could be released from an additional burden of care of their shoulders in the middle-to-long term.
However, most importantly, by using these “health maintenance” technologies themselves, women could remain healthy and youthful for longer. After all, when most of us look in the mirror, we would prefer to see shining soft skin, youthful fitness, and the smile of a woman enjoying her life to the fullest at any age!