Your #1 Source for Life Extension News
lifespan.io offers the latest information on rejuvenation biotechnology and life extension technologies. Our news outlet brings you the latest aging research, financial, and advocacy news, which is great if you like to keep up to date with everything happening in this rapidly changing field on a daily basis.
The Latest Longevity News Stories

Preventing Load-Induced Arthritis at the Cellular Level
Researchers have discovered that the osteoarthritis-inducing effects of excessive mechanical stress can be mitigated by increasing miR-330, a key regulator in cartilage and bone cells. Backbreaking labor is exactly that […]

The Thalion Initiative: A New Non-Profit With Big Ambitions
The longevity field remains small and starved for resources, especially the subfield devoted to the fundamental biology of aging, despite near-universal agreement that solving aging requires understanding it first. With VCs looking […]

Rejuvenation Roundup May 2026
Approaches that modify the processes of aging at their roots have gone well beyond basic research and into therapies intended for the clinic within the next few years. Here’s how the […]

Harvard Publishes a Longevity Report for the General Public
The report, titled “Pathways to Longevity”, introduces several important longevity concepts to the general reader and is another sign that the field is coming of age and entering the mainstream. People do […]

A Better Algorithm for Predicting How Cells Behave
In a preprint published in arXiv, researchers from Altos Labs have described a machine learning algorithm that performs end-to-end prediction of how cells’ gene expression will respond to interventions. The need […]
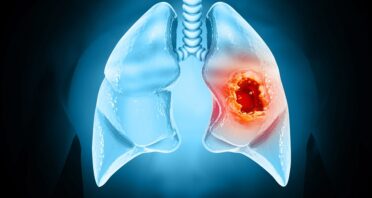
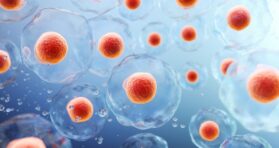
Early Cancer Cells Change Their Surroundings to Form Tumors
Scientists have demonstrated how cancer cells influence neighboring cells to create a favorable niche for the tumor to grow. This […]

Cardiovascular Health During the Menopausal Transition
A recent study compared premenopausal, perimenopausal, and postmenopausal women’s cardiovascular health. Perimenopausal women had about twice the odds of having a poor overall score when compared with premenopausal […]

Tau Protein Is Crucial for Encoding Long-Term Memory
Scientists have uncovered an unexpected function of the tau protein, which is mostly known for its role in Alzheimer’s and related disorders: […]

How Omega-3 Fatty Acids May Alleviate Kidney Disease
Researchers have discovered the role of cellular senescence in the interaction between omega-3 polyunsaturated fatty acids (PUFAs) and chronic kidney disease […]
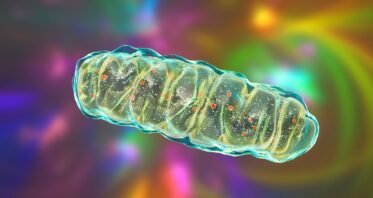
Mitochondrial Aging Linked to Losing Crucial Membrane Lipid
Scientists have found that the levels of phosphatidylcholine, the most abundant lipid in mitochondrial membranes, decline with age, driving mitochondrial aging in worms and possibly humans. Supplementing the lipid helped in an in vitro experiment […]
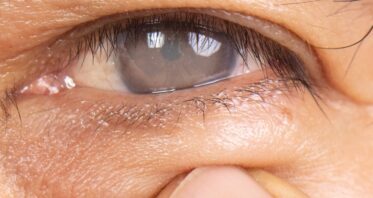
How an Oxidative Stress Regulator Makes Cataracts Worse
Researchers have outlined a key receptor and protein involved in the formation of cataracts, paving the way for potential treatments targeting them. Oxidative stress and cataracts are closely related Cataracts, which cloud the lenses of […]

Untangling Cellular Senescence at Its Roots
In Aging Cell, researchers have described the differences between primary and secondary senescent cells, comparing radiation-induced senescence to senescence induced by the senescence-associated […]
Interviewing the leading experts in aging research and longevity
We have a dedicated team of journalists who have interviewed many of the leaders in the field about their research and the drive to end age-related diseases. You can find our latest interviews below.
Regular Digest Articles
We publish the Rejuvenation Roundup – a monthly digest of what is happening in the field, a Longevity Market Recap – a monthly digest focused on the investment and business side of the field, and a quarterly Editorial – focusing on the activities of the news outlet and the wider organization.
Industry Press Releases
You can find some press releases from various companies in our field below. lifespan.io does not endorse any of these PRs and they are simply provided for information and interest.
Want even more news?
If you want to see even more recent articles, check out all news stories, or if you would like to look at a specific year or month head to the news archive.