Your #1 Source for Life Extension News
lifespan.io offers the latest information on rejuvenation biotechnology and life extension technologies. Our news outlet brings you the latest aging research, financial, and advocacy news, which is great if you like to keep up to date with everything happening in this rapidly changing field on a daily basis.
The Latest Longevity News Stories
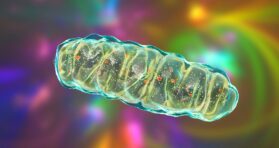
Mitochondrial Aging Linked to Losing Crucial Membrane Lipid
Scientists have found that the levels of phosphatidylcholine, the most abundant lipid in mitochondrial membranes, decline with age, driving mitochondrial aging in worms and possibly humans. Supplementing the lipid helped in an in […]
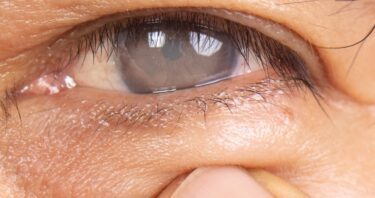
How an Oxidative Stress Regulator Makes Cataracts Worse
Researchers have outlined a key receptor and protein involved in the formation of cataracts, paving the way for potential treatments targeting them. Oxidative stress and cataracts are closely related Cataracts, which cloud the lenses of […]

Untangling Cellular Senescence at Its Roots
In Aging Cell, researchers have described the differences between primary and secondary senescent cells, comparing radiation-induced senescence to senescence induced by the senescence-associated secretory phenotype (SASP). Heterogeneity on top of heterogeneity It is well-known that senescent […]
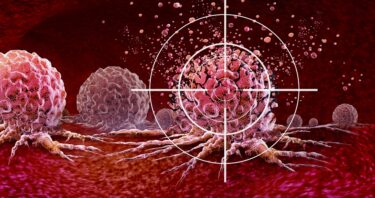
CRISPR-Based System Targets RNA and Kills Cells on Demand
Scientists have devised a CRISPR-based tool that can kill cells carrying a specific strand of RNA. The tested targets include cancerous and virus-infected cells [1]. Targeted assassination of cells CRISPR-based systems work by cutting or changing DNA […]

Developing a Drug To Reverse Heart Disease
We have spoken with Reason from Repair Biotechnologies about his company’s lead candidate, REP-0004, a drug targeting the liver to reduce excess intracellular free cholesterol. The FDA has […]
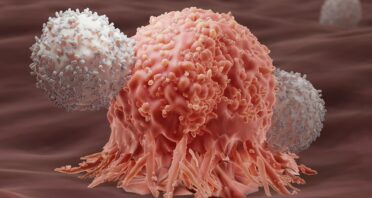
New mRNA Therapy Destroys Cancer by Improving T Cell Priming
Scientists have found a way to drastically ramp up mouse immune responses to cancer along with flu and COVID-19 [1]. How to […]

Matthew O’Connor on Cyclarity’s Successful Phase 1 Trial
Most cardiovascular trials focus on lowering LDL cholesterol or reducing inflammation to slow disease progression. UDP-003 targets the root cause: toxic 7-ketocholesterol (7KC) inside macrophages and soft plaques. It […]

Current Clinical Trials of Alzheimer’s Drugs
This month, a group of researchers published an annual report on the clinical trials that are testing drugs for Alzheimer’s disease. Overall, they reported an increase in the number of trials, […]
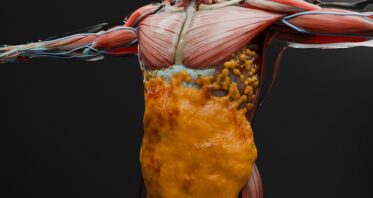
GLP-1 Drugs’ Muscle Effects Similar to Ordinary Weight Loss
A new study suggests that GLP-1 receptor agonists do not affect muscle mass any more than weight loss caused by caloric restriction, and this appears […]

Junyue Cao on How the Body Ages, Cell by Cell
Dr. Junyue Cao is a professor at the Rockefeller University, and his lab develops ultra-high-throughput single-cell technologies and applies them to the biology of aging. In a recent paper published in […]
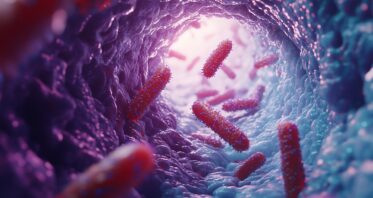
How Intestinal Aging Encourages Harmful Bacteria
In Aging Cell, researchers have elucidated the relationship between intestinal aging and age-related changes to the gut microbiome. Two interdependent biologies The human gut works through the interaction of two entirely different sets of cells. The first is […]

Creatine Shows Synergy With Exercise in Older Adults
In a new study, the popular supplement creatine seemed to add to some of the beneficial effects of power training [1]. […]
Interviewing the leading experts in aging research and longevity
We have a dedicated team of journalists who have interviewed many of the leaders in the field about their research and the drive to end age-related diseases. You can find our latest interviews below.
Regular Digest Articles
We publish the Rejuvenation Roundup – a monthly digest of what is happening in the field, a Longevity Market Recap – a monthly digest focused on the investment and business side of the field, and a quarterly Editorial – focusing on the activities of the news outlet and the wider organization.
Industry Press Releases
You can find some press releases from various companies in our field below. lifespan.io does not endorse any of these PRs and they are simply provided for information and interest.
Want even more news?
If you want to see even more recent articles, check out all news stories, or if you would like to look at a specific year or month head to the news archive.