What are B Cells? A Summary of B Lymphocytes
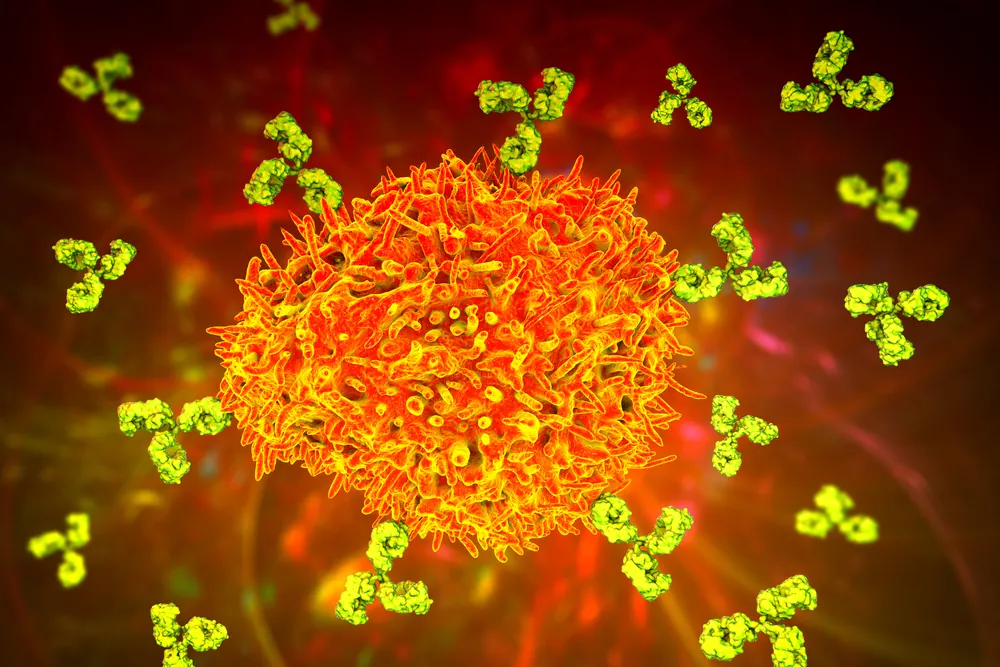
B cells (the precursors to plasma cells) are a type of white blood cell and the source of antibodies within the body. These antibodies have immunological, scientific, commercial, and industrial uses and are a major part of our ability to carry immunity.
What are B cells?
B cells are one of the two types of lymphocytes, white blood cells, the other kind being T cells. They are also known as B lymphocytes and are an important part of our immune system.
The immune system as a whole can be broadly separated into two main branches: the innate immune response and the adaptive immune response. The innate immune response is performed by a system that is always present across the body. The adaptive immune response appears only in response to an infection and is always specific to a particular infectious agent.
B cells are part of the humoral immune response and a part of the adaptive immune system and can only impact extracellular threats, meaning outside of our cells.
Where are B cells produced?
B cells are created by the hematopoietic stem cells located in the bone marrow. They develop in the bone marrow or within the lymph nodes before becoming mature B cells.
Many people assume that these get their name due to being produced in the bone marrow. However, the “B” actually comes from the Bursa of Fabricius in birds, a specialized lymphoid organ essential for B cell development in birds. The closest equivalent in humans is probably the tonsils or lymphoid tissue in the intestine.
What do B cells do?
The B cell functions to fight infections from bacteria and viruses. Like most immune cells, B cells have a very specific function: the production of Y-shaped proteins called antibodies. These play a major role in immunity.
In order for B cells to produce antibodies they must first become activated B cells. T cells are required for the activation of B lymphocytes, which interconnects two major parts of the immune response.
What are antibodies?
Antibodies, otherwise known as immunoglobulins, are water-soluble proteins that the human body uses to fight large, external threats, such as parasites and bacteria, that cannot hide within our own cells.
There are five main types of antibody:
| IgE | Defense against helminth worms (and cause of the side effect of allergies). |
| IgA | General, found in mucus, saliva, breast milk, blood, and tears. |
| IgG | Anti-bacterial and anti-virus, found in all tissues of the body. These are some of the few antibodies that can cross a mother’s placenta without causing damage to the offspring. There are multiple types of this kind. |
| IgM | Found in blood and lymph, first to be made in response to infection, involved in the B cell activation process. |
| IgD | Involved in the B cell activation process. |
What do antibodies do?
Antibodies can weaken or kill harmful pathogens (infectious agents) directly, but there are other uses for them.
They can be used to clump pathogens together in a process known as agglutination, making it easier for macrophages and other immune cells to target them. This ability to clump pathogens together has a valuable scientific and diagnostic use too. If a cell is infected by a virus or has a specific receptor on its surface, an antibody specific to that virus or receptor can be used to bind these cells together.
Normally, if you take a group of cells suspended in water and leave them for a while, they will sink to the bottom of their container, leaving a ‘dot’. If they are bound together by antibodies, they will instead form a ‘matrix’ within the water, essentially remaining suspended in the water. With this a scientist can estimate the concentration of viruses in any sample by detecting how much antibody is needed to prevent the formation of a ‘dot’.
Antibodies are a key method by which the body maintains immunity to specific diseases. Immunity against bacteria mainly relies on antibodies and can be seen through the primary and secondary immune response. The primary immune response is the immune response to the first infection from a specific pathogen, while the secondary immune response is the immune response to an infection by the same pathogen a second time.
During the secondary immune response, the concentration of antibodies in the bloodstream increases much more rapidly after an infection compared to the primary immune response. This is due to the presence of T and B memory cells that remember the pathogen and activate the immune response more quickly; this is of major significance to the immune system and how it responds to threats.
Chemical signals involved in the creation of antibodies
The plasma cells know what kind of antibody to make through exposure to particular chemical messengers[2]. Interleukins (ILs), interferons (IFN), transforming growth factor (TGF), and these factors do the following:
| IL4 | Signals the creation of IgE and IgG1. |
| IL4, 2 and 5 | Signal the creation of IgM. |
| IFN | Signals the creation of IgG2a and IgG3. |
| TGFbeta | Signals the creation of IgA and IgG2b. |
| IL4 and IL10 | Signal the creation of IgD, though IgD can be made spontaneously. |
There are many types of antibodies, each with different purposes, which are created in response to chemical signals.
How B cells produce antibodies
In order for a B cell to start producing antibodies, a very specific sequence of events must happen. First, an infectious agent, such as a bacterium, must enter the body. Next, a piece of the infectious agent’s machinery, such as a protein, must be visible on the surface of the infectious agent; this is where major histocompatibility complex (MHC) class molecules come in.
MHC class molecules come in two primary forms, MHC1 and MHC2, which are found on the cell surface of all nucleated cells in the human body.
In the case of viruses, these stick to a cell’s MHC1 receptor. Some viruses inhibit production of MHC1, which has led the human body to destroy any cell that does not show MHC1 on its surface.
At this point, the protein detected on the surface of the infectious agent can be called an antigen. If the infectious agent is killed by the innate immune response, the protein can be recovered in a number of ways; macrophages, for instance, can grab the antigens after consuming an infectious agent and present them on their surface MHC2 receptors.
Some antigens become free-floating after infectious agents have been destroyed. Dendritic cells can ‘taste’ these free-floating antigens and latch onto them, ready to present them. Dendritic cells can also phagocytose (engulf) infectious agents and destroy them particularly slowly, ensuring that they can collect antigens without destroying them[1]. With viruses, the protein stuck to the infected cell’s MHC1 receptor is automatically presented. Cells that present antigens on their surfaces are known as ‘Antigen Presenting Cells’.
B cell activation
 Next, to cause activation, the antigen on the MHC of the antigen presenting cell must be detected by a T cell using the T cell’s TCR receptor, while the T cell’s CD28 receptor must detect a B7 receptor on the antigen-presenting cell’s surface, which allows the T cell to realize that the antigen-presenting cell is native to the body.
Next, to cause activation, the antigen on the MHC of the antigen presenting cell must be detected by a T cell using the T cell’s TCR receptor, while the T cell’s CD28 receptor must detect a B7 receptor on the antigen-presenting cell’s surface, which allows the T cell to realize that the antigen-presenting cell is native to the body.
Either a memory T cell (which stores information vital to immunity) or a naive T cell (which is used for new threats) can be activated in this way. Because all T cells are specific to a single surface protein, only some T cells can be activated by any one antigen; these activated cells have been ‘clonally selected’.
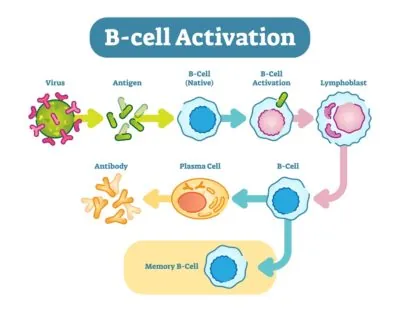
The selected T cells become active T helper cells before they begin to massively replicate in a process called clonal expansion. At the same time, a B cell is similarly activated by detecting an antigen on its surface through use of a specific, pre-prepared antibody. However, this will have no effect until a T helper cell brushes against the B cell and binds to its MHC, along with the usual CD28 – B7 binding to recognize the B cell as ‘self’. At this point, the T helper cell releases cytokines – chemical messengers (IL4 specifically) – which are detected by the B cell, causing its activation.
Once a naive B cell is activated, it begins to clonally expand as well, dividing multiple times and specializing (differentiating) the resulting ‘daughter cells’ into either plasma cells or memory B cells. The memory B cells are kept in order to maintain immunity, while the plasma cells begin to produce antibodies, releasing them into surrounding tissues and the blood. Memory B cells can circulate in the bloodstream in a dormant state, sometimes for decades before they activate.
The difference between B cells and T cells
Just the same as T-cells, every B cell has a receptor that only connects to one antigen shape. And much like T-cells, B-cells that recognize self-antigens are destroyed. This is so they don’t start attacking your healthy cells and destroying them.
A key difference between T cells and B cells is that B cells are able to connect to antigens directly on the surface invading virus or bacteria. T-cells can only connect to virus antigens on the outside of infected cells. In other words, B cells attack invaders outside the cell, while T cells attack infected cells.
B cells and T cells work together to keep us healthy and safe from invading pathogens. In many ways, the immune system can be considered our very own “living medicine” and technologies are being developed currently to improve the efficiency of these and other types of immune cells to help combat diseases such as cancer.
Literature
[1]Savina, A., & Amigorena, S. (2007). Phagocytosis and antigen presentation in dendritic cells. Immunological Reviews, 219(1), 143-156. https://dx.doi.org/10.1111/j.1600-065x.2007.00552.x
[2] Levan-Petit, I., Lelievre, E., Barra, A., Limosin, A., Gombert, B., Preud’homme, J., & Lecron, J. (1999). Th2 cytokine dependence of IgD production by normal human B cells. International Immunology, 11(11), 1819-1828. https://dx.doi.org/10.1093/intimm/11.11.1819