A high-quality, randomized, controlled trial found no effect of vitamin D supplementation or blood levels on the incidence of fractures in an aging population [1].
The common perception doesn’t match the science
It’s a long-held aphorism that vitamin D is good for bone health. This has been popular since it was discovered to be a cure for rickets, the child-specific form of osteomalacia (bone softening). Today, many products aimed primarily at children, such as milk and breakfast cereals, are fortified with vitamin D, which has also become a very popular supplement among adults. This includes many people in the longevity field, as age-related osteoporosis is a genuine concern, especially among women [2]. Some enthusiasts even advocate for vitamin D “mega-dosing”.
As the authors of this new study note, between 1999 and 2012, the use of vitamin D supplements increased from 5.1% to 19% among U.S. adults. However, scientists have been unable to confirm any positive effects of vitamin D supplementation except for preventing rickets and osteomalacia in high-risk groups [3].
Robust design
Several years ago, an extensive VITAL trial was commenced to study the health effects of vitamin D supplementation on cancer and cardiovascular disease. Almost 26 thousand men older than 50 and women older than 55 were enrolled. The results, however, were disappointing: vitamin D showed no significant effects on any of the endpoints [4]. This latest ancillary study used VITAL’s database to look for possible correlations between vitamin D supplementation and bone health, which is exactly where vitamin D is supposed to shine.
The study design was considerably robust. For instance, it included a three-month placebo-only run-in to identify participants who were reliably taking their pills at home. Only compliant participants were included in the actual study. The researchers also controlled for confounding variables that could independently affect bone health. The participants were not stratified by their baseline vitamin D levels, meaning that both people with healthy levels of vitamin D and those with vitamin D deficiency were included.
Current recommended daily vitamin D consumption varies from 800 to 2000 IU (international units), depending on which organization you ask. Participants in the study group were receiving 2000 IU daily to achieve mean vitamin D blood levels of 40 micrograms per liter, which is on the higher end of the current recommendations. Incidence of bone fractures was chosen as the primary endpoint, and the median follow-up was 5.3 years.
D for disappointment
Mean vitamin D levels increased from 29.2 to 41.2 micrograms per liter in the study group while decreasing from 30.0 to 29.4 micrograms per liter in the placebo group. However, this did not lead to any statistically significant effect on most endpoints. Suprisingly, none of the vitamin D thresholds (<12, <20, <30, or ≥50 micrograms per liter) significantly influenced the effect – or, rather, the lack thereof.
Patients with abnormally low, abnormally high, or normal levels of vitamin D in blood serum were equally prone to first-time as well as recurrent fractures. There was also no effect modification by baseline age, sex, race or ethnic group, BMI, or personal use of supplemental calcium. Notably, the same group, also working on VITAL data, previously found that vitamin D supplementation did not affect incident fall risk or changes in bone mineral density or structure [5].
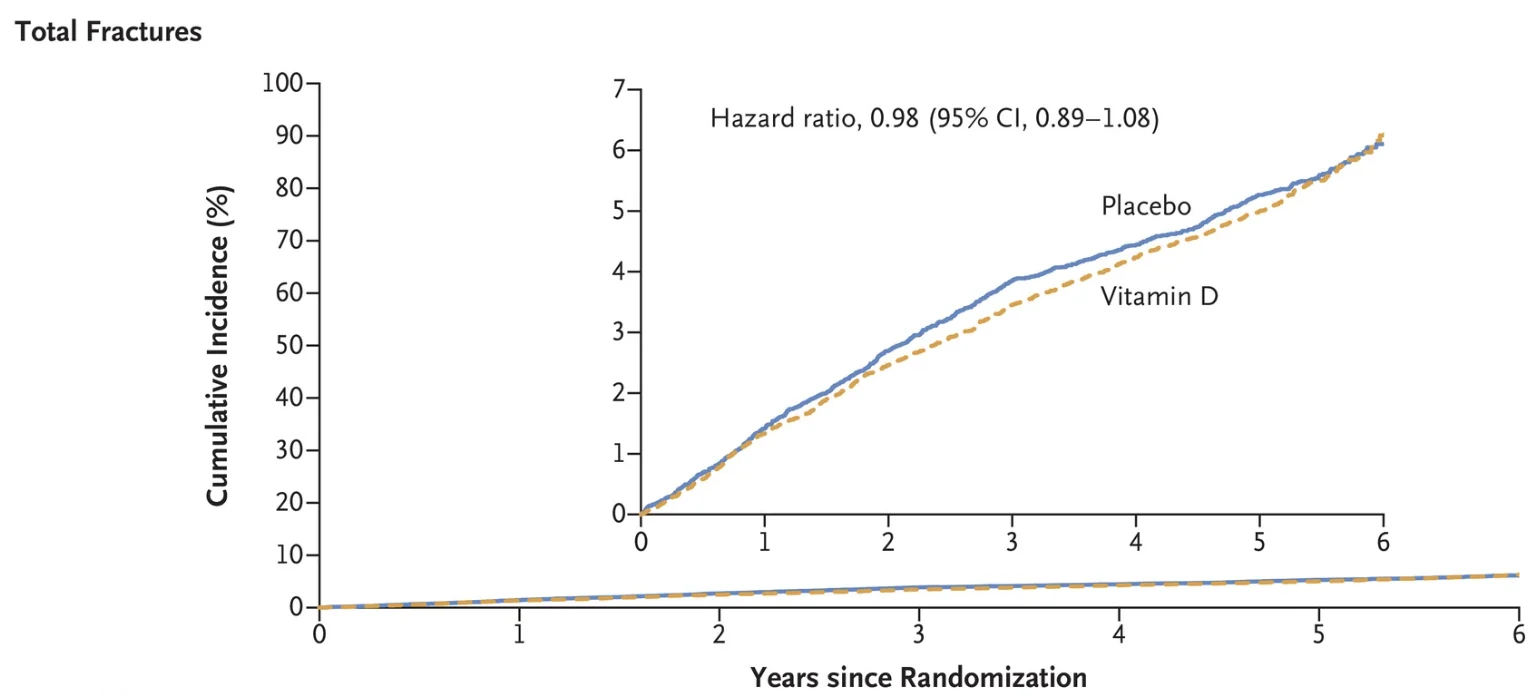
Among 25,871 participants (50.6% women [13,085 of 25,871] and 20.2% Black [5106 of 25,304]), we confirmed 1991 incident fractures in 1551 participants over a median follow-up of 5.3 years. Supplemental vitamin D3, as compared with placebo, did not have a significant effect on total fractures (which occurred in 769 of 12,927 participants in the vitamin D group and in 782 of 12,944 participants in the placebo group; hazard ratio, 0.98; 95% confidence interval [CI], 0.89 to 1.08; P=0.70), nonvertebral fractures (hazard ratio, 0.97; 95% CI, 0.87 to 1.07; P=0.50), or hip fractures (hazard ratio, 1.01; 95% CI, 0.70 to 1.47; P=0.96). There was no modification of the treatment effect according to baseline characteristics, including age, sex, race or ethnic group, body-mass index, or serum 25-hydroxyvitamin D levels. There were no substantial between-group differences in adverse events as assessed in the parent trial.
Conclusion
This meticulous study is a great illustration of how deceptive “common knowledge” can be. While many signs had pointed to vitamin D being essential for bone health, studies have repeatedly produced inconclusive results, and this new study, due to its robust design and large sample size, might be the last nail in the myth’s coffin. While it is still possible that vitamin D supplementation conveys certain health benefits (although benefits for CVD and cancer have also been all but ruled out), if you want to keep your bones strong as you age, you probably should look elswhere, such as at resistance training [6]. As for mega-dosing, some previous research suggests that it can actually be bad for you [7].
Literature
[1] LeBoff, M. S., Chou, S. H., Ratliff, K. A., Cook, N. R., Khurana, B., Kim, E., … & Manson, J. E. (2022). Supplemental Vitamin D and Incident Fractures in Midlife and Older Adults. New England Journal of Medicine, 387(4), 299-309.
[2] Li, G., Thabane, L., Papaioannou, A., Ioannidis, G., Levine, M. A., & Adachi, J. D. (2017). An overview of osteoporosis and frailty in the elderly. BMC musculoskeletal disorders, 18(1), 1-5.
[3] Reid, I. R., Bolland, M. J., & Grey, A. (2014). Effects of vitamin D supplements on bone mineral density: a systematic review and meta-analysis. The Lancet, 383(9912), 146-155.
[4] Manson, J. E., Cook, N. R., Lee, I. M., Christen, W., Bassuk, S. S., Mora, S., … & Buring, J. E. (2019). Vitamin D supplements and prevention of cancer and cardiovascular disease. New England Journal of Medicine, 380(1), 33-44.
[5] LeBoff, M. S., Chou, S. H., Murata, E. M., Donlon, C. M., Cook, N. R., Mora, S., … & Manson, J. E. (2020). Effects of supplemental vitamin D on bone health outcomes in women and men in the VITamin D and OmegA‐3 TriaL (VITAL). Journal of Bone and Mineral Research, 35(5), 883-893.
[6] Howe, T. E., Shea, B., Dawson, L. J., Downie, F., Murray, A., Ross, C., … & Creed, G. (2011). Exercise for preventing and treating osteoporosis in postmenopausal women. Cochrane database of systematic reviews, (7).
[7] Sanders, K. M., Stuart, A. L., Williamson, E. J., Simpson, J. A., Kotowicz, M. A., Young, D., & Nicholson, G. C. (2010). Annual high-dose oral vitamin D and falls and fractures in older women: a randomized controlled trial. Jama, 303(18), 1815-1822.




